Research
Engineering the fetal membranes with bioinspired materials
| Principal investigator: | Tina CHOWDHURY |
| Co-investigator(s): | Anna David and Jan Deprest |
| Funding source(s): | Prenatal Therapy Charity |
| Start: 01-12-2018 / End: 01-10-2028 |
Every year in the UK, an estimated 1 in 9 babies are born preterm because the fetal membranes (FM) spontaneously rupture too early. This condition is called preterm premature rupture of the fetal membrane (PPROM) and is a common cause of preterm birth. Increasingly also clinicians are treating babies in the womb using fetoscopic and open hysterotomy approaches. However, PPROM complicates over 40% of such surgeries leading to preterm birth in treated babies, reducing the clinical effectiveness of fetal surgery. There are currently no clinical solutions to improve healing of the FM after surgery or after it ruptures spontaneously.
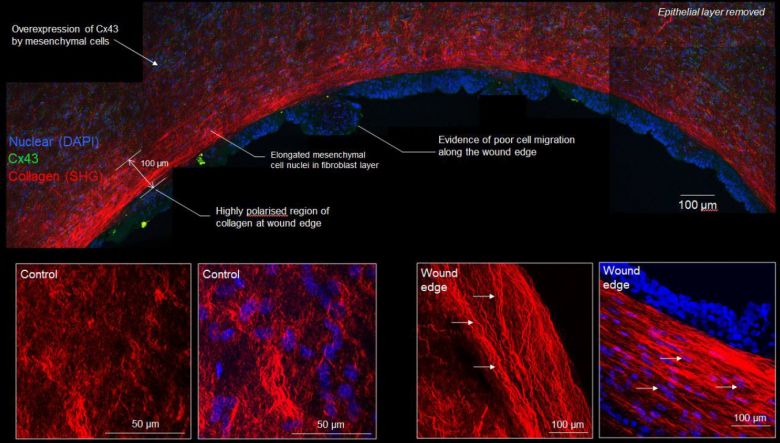
Our research has found a reason for this poor healing. Repeated stretching of the amniotic membrane, similar to the mechanical forces that occur in preterm labour, increases the levels of a protein called connexin 43 (Cx43) and prostaglandins, representing important inflammatory factors causing PPROM. We observed high levels of Cx43 in the amniotic membrane around the defect site after keyhole fetoscopic surgery. High Cx43 is known to delay healing of chronic skin wounds by preventing cell migration. We believe that in the amniotic membrane, elevated Cx43 prevents cells from crawling to the wound edge where they would normally produce collagen that builds structural bridges and repairs the defect. To encourage repair, we are developing materials that can rebuild the damaged tissue with collagen and elastin. We plan to integrate this membrane with a clinically approved therapeutic agent that will reduce Cx43 and stimulate repair of the defect.

